When to See a Spine Specialist for Low Back Pain: A Houston PT’s Guide
Most people with low back pain follow the same frustrating path: urgent care, primary care, maybe a chiropractor, eventually an MRI, sometimes a steroid injection, and only after months of bouncing around do they end up with someone who actually knows what to do with a spine.
The system isn't built to get you to the right person quickly. So this article is going to do something the system doesn't: help you figure out, in plain language, when to see a spine specialist for back pain — and when you don't need one at all.
I'm Dr. Sean Harris, a Doctor of Physical Therapy with a PhD in rehabilitation science, board-certified in orthopedics (OCS), and a Fellow of the American Academy of Orthopaedic Manual Physical Therapists (FAAOMPT). I've spent my career evaluating and treating spines. Here's what I tell my patients.
First: What is a "spine specialist"?
The term gets thrown around loosely. It can mean any of these people, and they do very different things:
Spine surgeon (orthopedic surgeon or neurosurgeon with spine fellowship) — performs surgery on the spine. Decompressions, fusions, discectomies. Does not typically manage conservative care.
Physiatrist (PM&R physician) — non-surgical spine medicine. Often performs spinal injections, manages medications, coordinates care.
Orthopedic spine specialist (non-surgical) — diagnoses spine conditions, orders imaging, often refers to PT.
Spine-focused physical therapist — diagnoses the movement-based source of the pain, builds a recovery plan, treats hands-on. No imaging, no injections, no medications.
Chiropractor — manual treatment focused on spinal manipulation. Quality varies enormously by individual.
For most people with low back pain, the right starting point is not a surgeon. About 90% of low back pain resolves with conservative care, and most of the remaining 10% gets diagnosed correctly with a thorough clinical exam — no MRI required up front.
Red flags: when to skip everything and go to the ER
Before we talk about anything else, you need to know the conditions where you don't ask questions, you go straight to an emergency department or call your doctor's office same-day. These are uncommon but serious:
Loss of bladder or bowel control (new onset)
Numbness in the saddle area (between your legs, around your genitals or inner thighs)
Progressive weakness in one or both legs that's getting worse over hours or days
Severe back pain after a significant trauma (car accident, fall from height)
Back pain plus fever, unexplained weight loss, or night pain that doesn't ease with rest
History of cancer with new back pain
These can signal cauda equina syndrome, spinal infection, fracture, or tumor. They're rare. But if you have one of them, the answer isn't a chiropractor or PT — it's the ER.
If none of those apply, keep reading.
The most common scenarios — and where to start
Scenario 1: Sudden onset back pain, no leg symptoms, no red flags
You bent over wrong, lifted something awkward, or woke up with it. Pain is in your back, maybe radiating into your buttock, but not down past the knee. No numbness, no weakness.
Where to start: A physical therapist who specializes in spines. Not a generalist, not a clinic that hands you to an aide for 45 minutes of stim and ice. You want someone who will actually examine you, identify the movement pattern that's irritating the tissue, and give you a plan you can execute.
Why not the surgeon or imaging first? Because most of these resolve in 2-6 weeks with the right plan, and imaging at this stage almost always shows incidental findings (degenerative changes, disc bulges) that aren't actually causing the pain but that scare patients into unnecessary procedures.
Scenario 2: Back pain with leg pain or numbness
The pain shoots into your leg, sometimes past the knee, sometimes into the foot. Maybe there's numbness or tingling. This is usually nerve root irritation — a "radiculopathy" in medical terms.
Where to start: Still a spine-focused PT first, in most cases. The exception is if you also have weakness in the leg (foot drop, can't push off your toes, knee buckling). Then you should be evaluated by a physician (orthopedic, physiatrist, or neurologist) in addition to starting PT.
A good PT can usually distinguish between a nerve being mechanically pinched (which often responds well to specific positions and exercises) versus a nerve that's chemically irritated by a fresh disc tear (which needs different treatment). Both are usually self-limiting with proper care.
Scenario 3: Chronic back pain, months or years
You've had this off and on for a long time. It's not getting better. You've maybe tried a few things — generic PT, chiropractic, massage, painkillers.
Where to start: A spine specialist who will spend an hour with you, ask about every previous treatment, identify what hasn't been tried, and rule out the structural diagnoses that get missed in 15-minute appointments. This is where a PhD-level evaluation matters — chronic pain is a different beast from acute pain, and it requires a different treatment philosophy.
In Houston, your cash-pay options are usually better than your insurance options here. Insurance-driven clinics typically can't afford to spend an hour with you on a first visit.
Scenario 4: Pain after a recent surgery or injection
You had a procedure and you're still in pain, or new pain. Go back to the surgeon or doctor who did the procedure first. They need to know, and they're the only one who can interpret what's happening with their work.
The 4-week test
Here's a rule that holds up across the literature: if you've had back pain for less than 4 weeks, no red flags, and you're doing the right things (movement, gradual loading, avoiding the specific provocations), you should be seeing improvement.
If you're at 4 weeks and nothing has changed, you have your answer. Time to escalate. That doesn't necessarily mean surgery — it means getting a deeper evaluation. A spine-focused PT can re-examine, an orthopedic or physiatrist can evaluate for imaging, and you have a clearer path.
If you're at 4 weeks and you're slowly getting better, keep going. Most spines just need time and the right inputs.
How to find the right spine specialist in Houston
If you've decided you need to escalate:
For a surgical evaluation, ask for an orthopedic spine surgeon or a neurosurgeon who is fellowship-trained in spine. Look for someone who is conservative — meaning they recommend surgery only when conservative care has clearly failed.
For a non-surgical workup, look for a physiatrist (physical medicine and rehabilitation). They handle the spine medically without going to the OR.
For physical therapy, you want someone with a Doctor of Physical Therapy (DPT) degree, board certification in orthopedics (OCS) or a fellowship credential (FAAOMPT), time (if they're seeing you for 20 minutes and giving you a printout, find someone else), and a specific approach to the spine — not generic exercises, but examination-driven, movement-specific treatment.
The truth most people don't hear
Most low back pain — even severe, even with sciatica — gets better. The body is more resilient than the diagnoses make it sound. Disc bulges heal. Nerve irritation calms down. Muscles strengthen. The data is overwhelming on this.
What matters is getting the right plan from the right person, early, before the pain becomes a chronic pattern. The expensive part of back pain isn't the right care up front — it's the wrong care that drags on for years.
If you're in Houston and you're trying to figure out where to start, we offer a free 15-minute screening call for exactly this reason. You'll talk to me directly, describe what's going on, and I'll tell you — honestly — whether physical therapy is the right starting point, whether you need a different specialist first, or whether your situation is simple enough that you can probably handle it on your own with the right information.
Schedule a free screening call
You don't need to bounce around the medical system for months. You need someone to tell you, in 15 minutes, where to start.
Dr. Sean Harris, PT, DPT, PhD, OCS, FAAOMPT, is the founder of Harris Institute for Rehabilitative Therapies in Houston, TX. He specializes in spine, sports, and orthopedic physical therapy with a focus on performance-based rehabilitation.
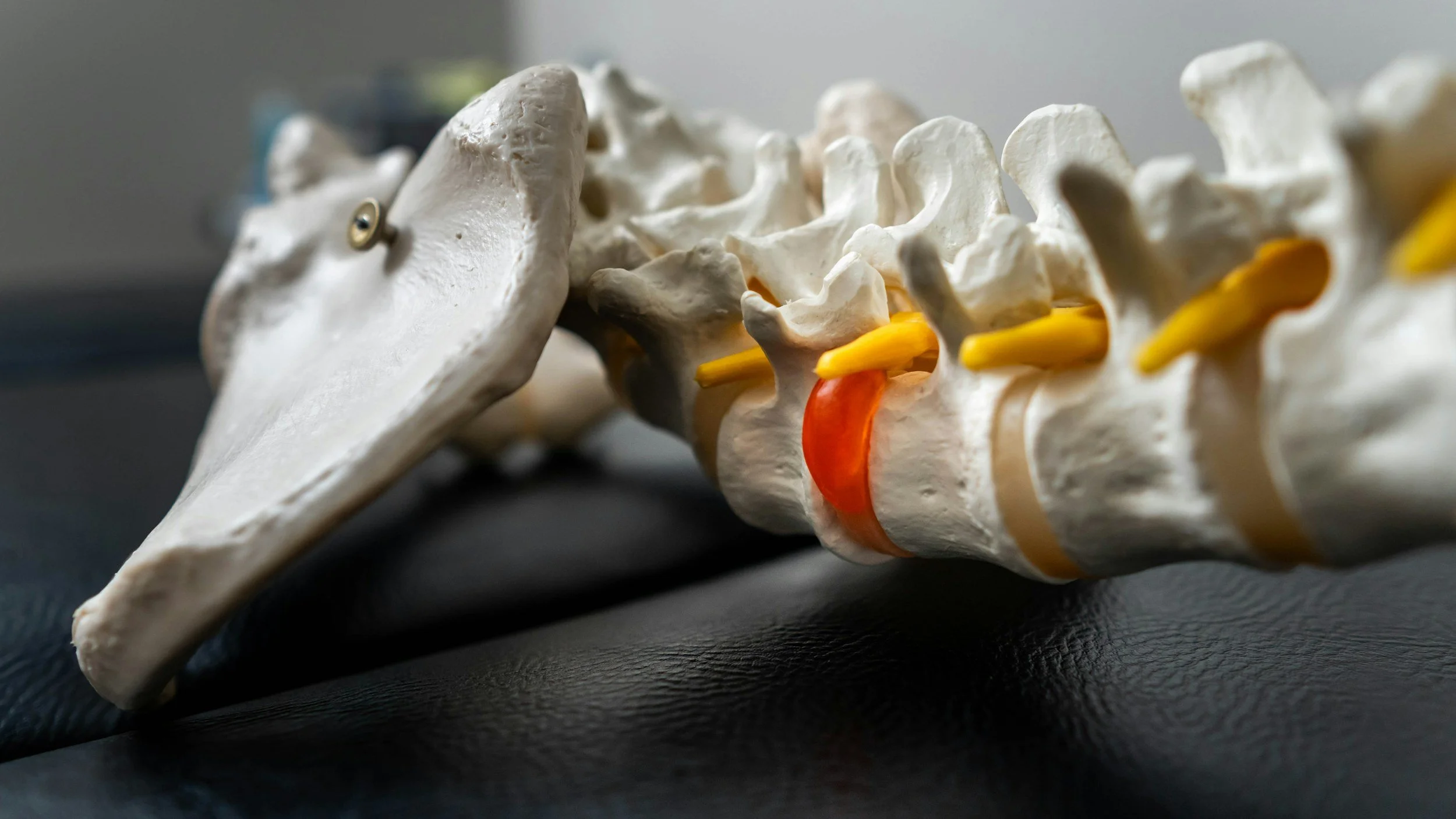
Spinal nerve roots are (shown here) are involved with radiculopathy and radicular pain
At the Harris Institute - we evaluate the differences between these nerve pathologies!